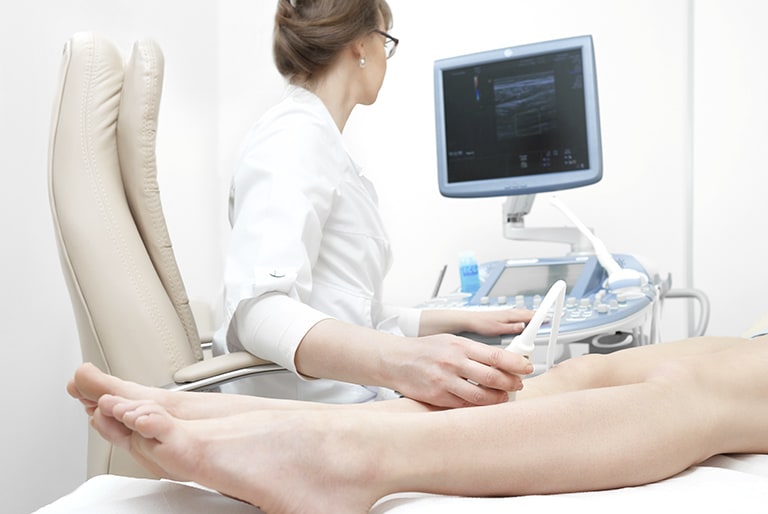
Lymphatic drainage
Your doctor will often prescribe lymphatic drainage against water retention in your legs and vein problems, in order to dissolve the accumulation of fluid and to stimulate blood flow. But what is that exactly and what happens during the treatment?
What is lymphatic drainage?
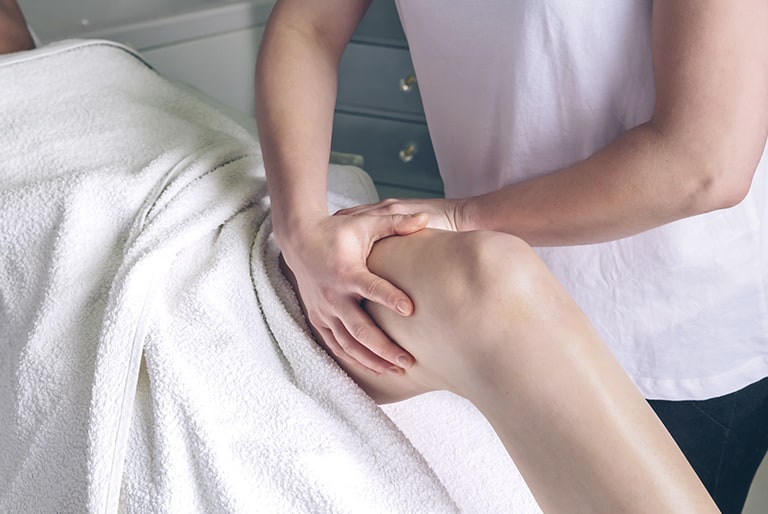
Normally, blood and lymph transport nutrients into the smallest vessels in your body tissue, and then flow through the blood and lymphatic channels together with the waste products. Nutrients in, waste out – several litres of fluid are in constant motion in your body.
But fluid collects in your tissue if there is a functional disorder in this process. Such accumulations of water can be dissolved and transported away through the gentle massaging of your lymph nodes and lymphatic channels. Usually lymphatic drainage is performed by specially-trained phlebologists, physiotherapists or masseurs. It is usually prescribed in addition to a compression therapy, which should prevent oedemas reappearing.In addition to that, taking medicines, known as oedema protective agents, like Veno SL® 300, helps to improve the fluidity of your blood and to counteract the build-up of water retention in your tissue. Regular exercise is also an important factor for the success of the therapy.
When does lymphatic drainage make sense?
If water is retained in the tissue in your arms or legs, lymphatic drainage can stimulate the stagnated lymph flow. The therapy is recommended against the following symptoms:
- Swollen legs
- Heavy legs
- Water in the legs
- Lymphoedema
- Lipoedema
- Weak veins
- Varicose veins
- Water retention during pregnancy
- Rheumatic diseases
- Arthritis
- Migraines
Lymphatic drainage is often prescribed after an operation, because the lymphatic channels can be severed during a surgical operation and water retention builds up due to medication and prolonged lying. Decongestion therapy supports the lymphatic system to operate.
What exactly happens during lymphatic drainage?
Manual lymphatic drainage (MLD) is performed by a therapist who massages the lymphatic channels on your arms and legs using special hand grips. Since there are numerous lymph nodes on your neck and collar bone which have an important function in the lymphatic system, this area will also be gently treated. The therapist activates lymphatic drainage through targeted movements and grips, which are done in a rhythmic, circular or pumping manner:
- Stationary circles
- Twist grip
- Scoop grip
- Pump grip
There is no pressure required, as with a conventional massage, because the lymphatic channels run close to the surface of the skin. The contact is soft and more like stroking. The treatment can last for between 30 and 60 minutes, depending on the prescription. A compression bandage is applied at the end in order to support the removal process and to prevent renewed swelling of the tissue.
Always have a specialist conduct the lymphatic drainage rather than do it yourself. Because if you massage at the wrong point and with too much pressure, you can damage your tissue.
What is complex decongestive therapy?
The term complex decongestive therapy (CDT) combines a whole therapy concept which basically comprises four important components:
- Compression therapy
- Lymphatic drainage
- Movement
- Skin care
The combination of the four building blocks has proven to be very successful to date in the treatment of lymphoedema.
How often should you have lymphatic drainage?
The length and frequency of decongestive therapy is dependent on the types of symptoms and is determined by your doctor. Lymphatic drainage should be carried out every day in the case of acute swellings and following operations, sometimes even more than once a day. Lymphatic drainage is an inherent part of the permanent therapy if there is chronic lymphoedema or lipoedema.
When should you not have lymphatic drainage?
Lymphatic drainage cannot be done if there is reason to suspect acute thrombosis, because the stimulated blood flow would propel the blood clot forwards and could lead to pulmonary embolism. Lymphatic drainage makes sense as a part of the subsequent therapy if the clot has been medically removed, in order to support the removal of the fluids and to prevent blockages.
Lymphatic drainage is also not recommended in the case of heart insufficiency, kidney weakness or acute infection. Discuss the therapy beforehand with your doctor; they are best situated to assess if lymphatic drainage is appropriate in your individual case.
Is the cost of lymphatic drainage covered by health insurance funds?
If the lymphatic drainage has been prescribed by your doctor as part of a therapy for venous diseases or oedemas, the health insurer covers the costs. There may be a supplementary charge. If the treatment is a voluntary preventive measure against water retention, then the patients usually have to bear the costs themselves. Consult your doctor about this beforehand and ask your health insurer directly if they will accept the costs.