Spider Veins: formation, treatment and prevention
A large portion of the population knows them, these web-like vein formations which are visible under the skin, predominantly on your legs. Many people see them as a beauty flaw, which they prefer to hide beneath trousers. But how are these bluish-red webs formed? And are spider veins even dangerous?
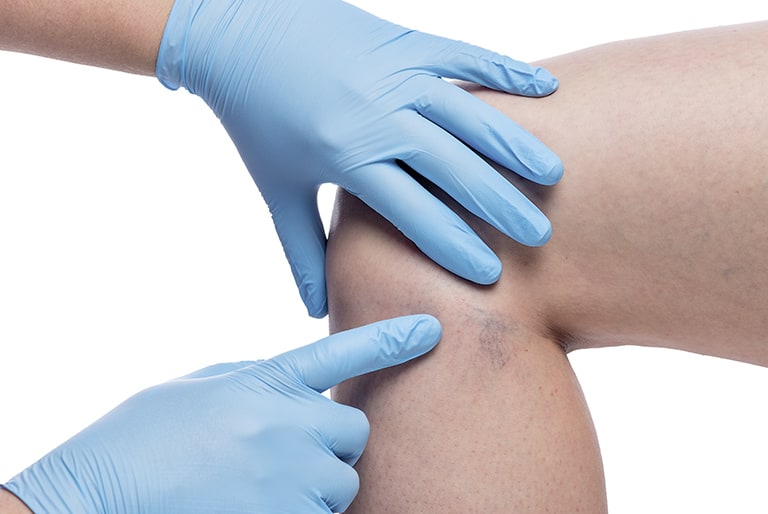
What are spider veins?
The fine webs sometimes pop up individually and are hardly noticeable. Sometimes certain parts of the body are more affected. In such cases, the spider veins appear at first glance to be a bruise, but on closer inspection, the tiny bluish-red veins are clearly recognisable.
They owe their name to the fine net-like patterns which look like a spider’s web. In the diagnosis, doctors refer to them as Telangiectasias.
How do you get spider veins?
One of the causes of spider veins is weak connective tissue, which in many cases is hereditary. The predisposition is usually passed on if one parent suffers from spider veins or varicose veins. If both parents are afflicted, then the probability increases that their children will also one day discover the unloved little blue-red veins. The connective tissue undergoes hormonal changes during puberty and pregnancy, which is why many women suffer from spider veins even at a young age.
Another risk factor is consistently high blood pressure. The vessel walls stretch due to the high pressure with which blood is pumped through the veins. Over time, that leads to the blood not being transported optimally through the vessel and simply sinking into the smallest veins. What can be seen through the skin from outside is the build-up of blood in the tiny feeder veins of the blood vessels.
Smoking and excessive alcohol consumption also lead to damage in the vessels, and thereby encourage the formation of spider veins and other vascular diseases.
How dangerous are spider veins?
In principle, spider veins are not dangerous and are more of a beauty flaw for the afflicted, which they would like to get rid of for cosmetic reasons. In contrast to varicose veins, they do not necessarily have to be treated or removed. Pain and circulation problems from spider veins are not normally something to be feared.
Only rarely are spider veins a warning signal for a serious illness of the deeper-lying veins. You should ask a doctor for advice if the unsightly venous webs appear suddenly or in increased numbers, just to be sure. They can examine the vein composition with the aid of an ultrasonic scan. The specialist doctor for veins is called a phlebologist.
What can I do to prevent spider veins?
Unfortunately, the formation of spider veins cannot be completely prevented. But there are several possible ways to promote healthy veins and to prevent spider veins from developing into varicose veins.
- Healthy lifestyle: a balanced, vitamin-rich diet, moderate sport and the avoidance of stress are the basic requirements for healthy veins.
- Movement: regular movement boosts vein function. That is particularly true for people whose jobs require them to stand or sit a lot. In such cases, it is important to have short movement breaks in order to get the muscle pumps working. Briefly stretch your legs now and again, walk on the spot or integrate some foot gymnastics into your daily routine.
- Avoid excess weight: excess weight slows down the flow of blood through the veins. It also encourages vessel-damaging disorders such as high blood pressure.
- Hot and cold showers: switching between cold and hot water stimulates circulation and tightens connective tissue. Hot and cold showers are like training for your veins, which then become more elastic. Regular massages are equally as effective.
- No tight clothes: clothes which are too tight cause the blood to build up in your veins. Rather wear loose-fitting trousers and skirts, so that your blood can circulate freely.
- Put your feet up: put your feet up now and again in order to reduce the build-up of blood in your legs. That stimulates the flow of blood and helps against heavy, swollen legs.
- Compressions stockings: people who are particularly prone due to their parents can wear compression stockings as a precaution. They are also advisable for pregnant women, who have an increased risk of developing spider veins and varicose veins.
- Troxerutin: the active ingredient Troxerutin, contained in Veno SL® 300, is extracted from an ingredient of the Japanese Pagoda Tree. It improves the blood’s fluidity and hinders the formation of spider veins.
Spider veins increase in number as you get older, and that is why it is particularly important to pay attention at a young age to the health of your veins.
Can you have spider veins removed?
From a medical standpoint, you do not have to have spider veins medically removed, however people afflicted suffer from the small unsightly veins, which in summer are particularly visible when wearing short trousers and skirts. Anyone who wishes to have flawless legs can choose from several procedures:
- Sclerotherapy: this involves injecting a solution into the veins which leads to the walls of the veins sticking together. This prevents blood from circulating through the vessels and they fade over time.
- Laser therapy: fine spider veins can be removed by lasers. The targeted bundled light energy heats the blood in the vessels. That damages the small veins, their walls stick together and ideally the connective tissue structures are gradually absorbed by the body.
- IPL: treatment with a flash lamp has the same objective as laser therapy. The IPL method (intense pulsed light) is mainly used for spider veins spread over a large area.
As a rule, every process requires several sessions. In order to increase the chances of success of the treatment it is necessary to wear compression stockings afterwards. It is therefore best to plan to have the therapy during the colder months, in order to not have to wear the stockings during the summer.
As the removal of spider veins is a purely cosmetic procedure – you will usually have to bear the costs yourself. Make sure in advance that you are aware of what the costs are and whether you may qualify for some financial assistance.
Source: ¹ https://www.thieme-connect.de/products/ejournals/abstract/10.1055/s-0037-1617353